Mobile right heart thrombus and syncope
Three dimensional transesophageal echocardiography improves spatial location and relationship of lead-dependent infective endocarditis
16 Novembre 2020A 96-year-old female presented to the emergency room with shortness of breath following an episode of syncope at home. Examinations findings included moderate hypotension and jugular vein distension.
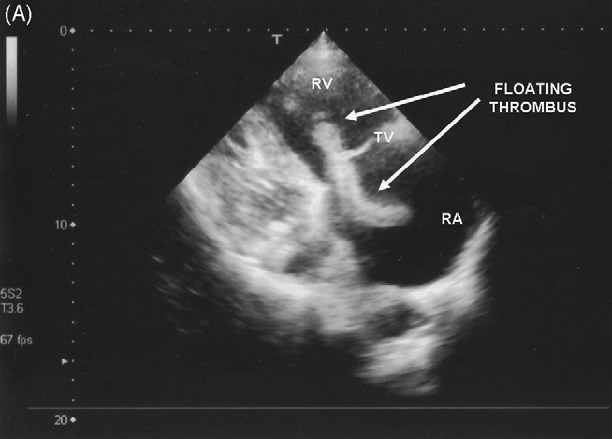
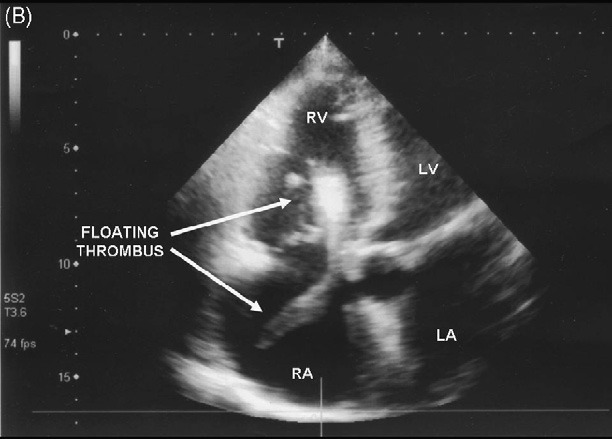
Blood gas analysis, whilst breathing room air, showed moderate hypoxaemia and hypocapnia. The patient’s initial care included high flow oxygen, intravenous access and monitoring. The ECG showed atrial fibrillation and incomplete left bundle branch block. Transthoracic echocardiography was performed immediately (see figure).
This showed a mobile large thrombus in the right heart chambers intermittently obstructing blood flow across the tricuspid valve (Panel A: 2 chamber apical view; B: 4-chamber apical view; RA: right atrium; RV: right ventricle; LA: left atrium; LV: left ventricle). After discussion of the treatment options (cardiac surgery, thrombolysis, intravenous heparin) with the patient and her family, an intravenous infusion of heparin was started. Unfortunately the patient’s condition deteriorated and she died shortly after her admission. Guidelines for the management of syncope1,2 recommend an extensive cardiac evaluation when the patient history, physical examination or ECG.